A Safe Space for Mental Health Healing
Innovative Mental Health Treatment Centers With Hundreds of 5-Star Reviews
Mental health impacts every aspect of life — emotions, relationships, and daily functioning. Our expert mental health programs offer personalized care, combining advanced treatments and holistic approaches to help you regain balance and well-being.
No matter your background or where you are in the process, we provide compassionate inpatient or outpatient support tailored specifically to you.
Common Conditions We Treat
- Anxiety Disorders
- Depression & Mood Disorders
- PTSD & Trauma-Related Conditions
- Self-Harm & Suicidal Ideation
- Borderline Personality Disorder (BPD)
- Dual Diagnosis & Co-Occurring Disorders



Most insurance plans cover treatment here, making the cost to you as low as possible - sometimes even zero.






Evidence-Based Mental Health Treatment Options
Having a wide range of proven and holistic therapies ensures each patient finds a combination of treatments that helps not just the mental health crisis, but their long-term mental wellness.
- Mental Health Disorders-Educational Programs
- Mindful-Based Cognitive Therapy (MBCT)
- Motivational Interviewing (MI)
- Psycho-Educational Therapy
- Trauma-Focused Therapies
- GeneSight Testing
- Transcranial Magnetic Stimulation (TMS)
- Spravato Ketamine Therapy
- Acceptance & Commitment Therapy (ACT)
- Cognitive Behavioral Therapy (CBT)
- Medication Management Treatment (MAT)
- Dialectical Behavior Therapy (DBT)
- Codependency Counseling
- Experiential Therapy
- Biomedical Feedback
- Eye Movement Desensitization and Reprocessing (EMDR)
Innovative Therapies Not Often Available at Other Treatment Centers
Despite growing clinical evidence, most mental health treatment centers are slow to adopt life-changing, innovative options. We are one of the few centers in the country to offer such a wide range of therapies and stay at the forefront of research.
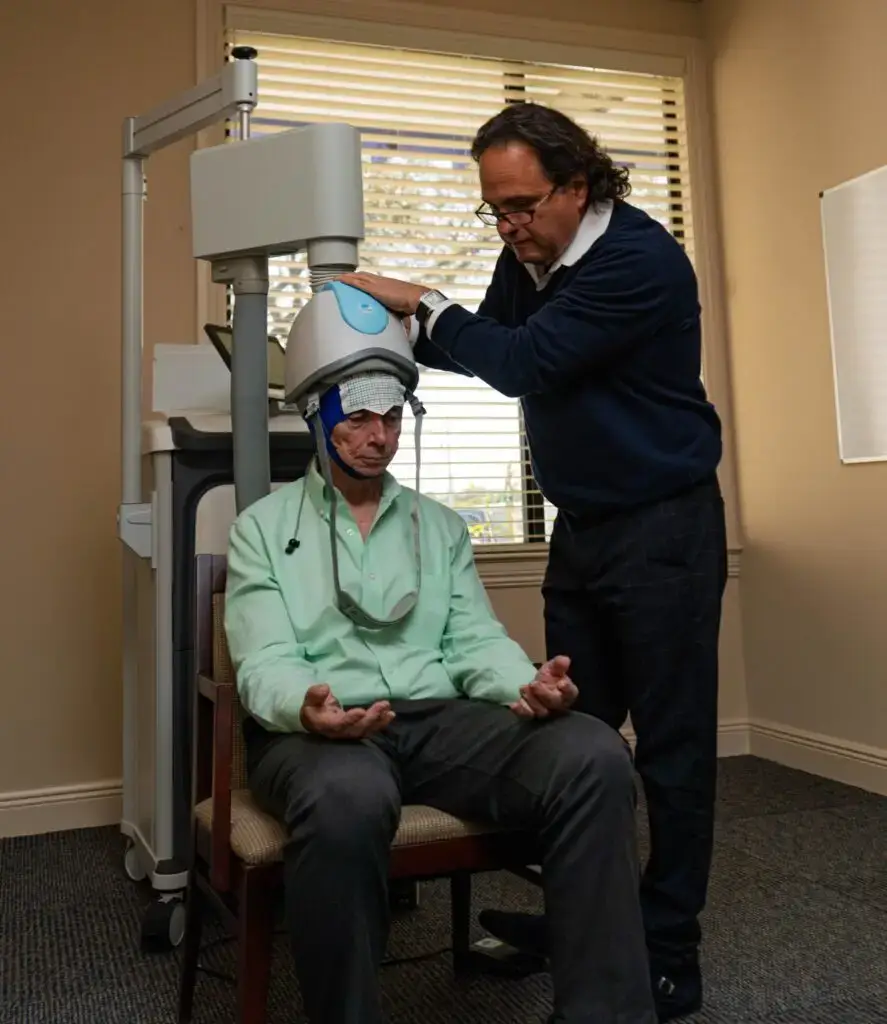
TMS Therapy
Using magnetic pulses to stimulate specific areas of the brain, TMS helps restore neural activity and improve symptoms when traditional treatments fall short. It’s a drug-free, well-tolerated option for mood disorders like depression.

EMDR Therapy
A highly effective non-invasive, drug-free therapy for PTSD, anxiety, and trauma-related disorders that uses guided eye movements to help reprocess distressing memories and relieve emotional distress.
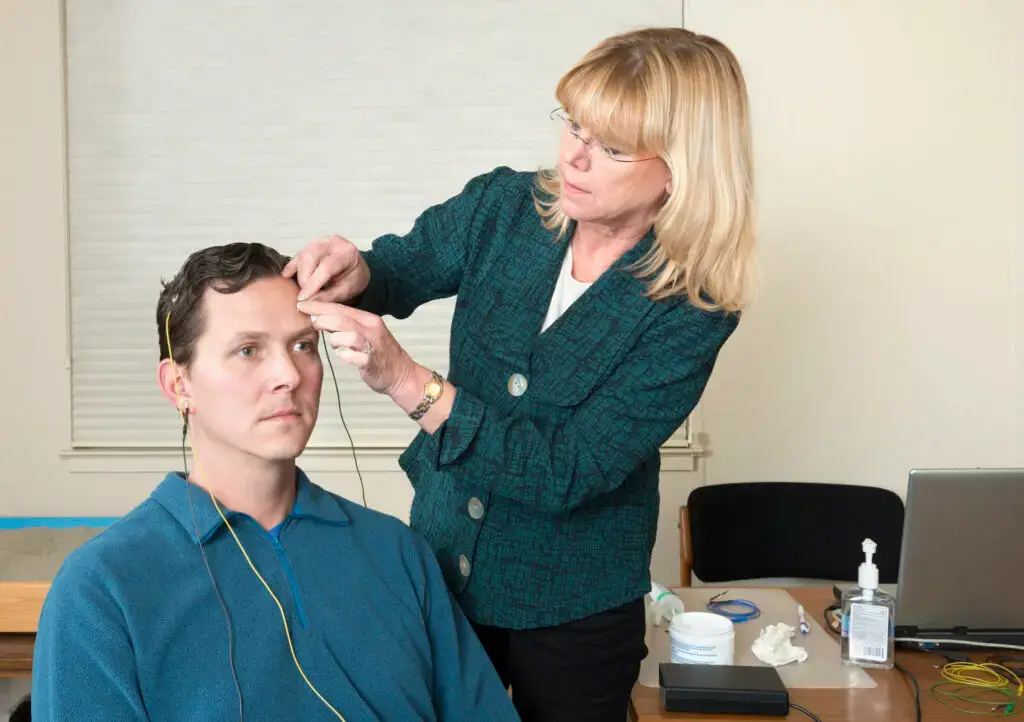
Biofeedback
A cutting-edge, drug-free therapy that uses real-time physiological data — like heart rate and brainwaves — to control anxiety and other mood disorders, regulate stress responses and improve overall emotional stability.

Spravato Ketamine Therapy
A breakthrough medication that is FDA-approved for effectively treating treatment-resistant depression. It can offer fast-acting relief, often within hours or days, when conventional treatments fail.
GeneSight Testing
Revolutionary genetic testing to tailor mental health medications based on your genes and metabolization, to reduce the time-consuming and frustrating trial-and-error guesswork of finding medications that actually work.
Holistic Mental Health Therapies
You are more than a diagnosis. Holistic therapies focus on treating the whole person—mind, body, and spirit—to promote lasting wellness beyond symptom relief. These therapies complement traditional treatments to provide a healthy outlet, reduce stress, and improve overall peace.
- Acupuncture
- Adventure Therapy
- Art Therapy
- Chiropractic
- Family Therapy Program
- Fitness & Nutrition
- Massage
- Meditation & Yoga
- Music Therapy
- Recreational Therapy
- Reiki Therapy
Backed by Hundreds of 5-Star Reviews
You’re not alone in this! Thousands of people have come to our mental health centers over the years feeling unsure recovery was possible. The true healing they found proves that change always is possible.
Five Addiction Treatment Center Locations
Whether you want to stay in the northeast or escape to sunny Florida, you’ll work with leading addiction specialists. All locations are safe, supportive and offer the innovative variety of therapies to keep you well long-term.
Available 24/7
The Next Step Is A Simple Phone Call
If you or a loved one is struggling with mental health, remember that hope is never lost. We believe in your strength and potential for a drug-free life.
Contact us for more information :
Call Us
(800) 817-1247
Verify Insurance
100% Confidential




